|
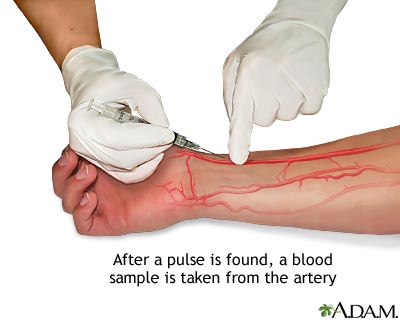
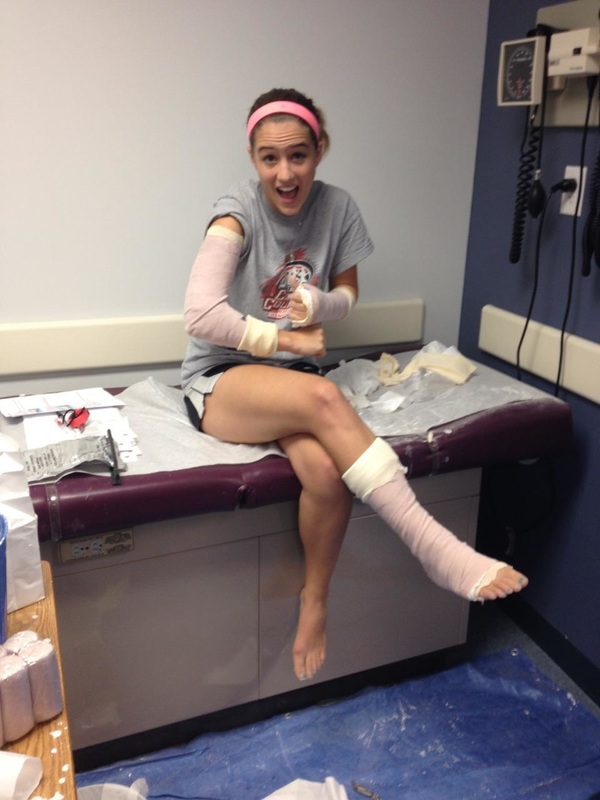
In clinical skills lab, we get to learn all the fun, hands-on things we will get to do as PA's. Today, we got to practice ABG's (Arterial Blood Gases) and splinting. Now, I have drawn hundreds and hundreds, maybe even near a thousand patients, but I have never done an ABG. The difference between an ABG and simple blood draws is that an ABG is arterial blood. The blood drawn for those colorful tubes and that IV giving you medications, is all venous blood. An ABG has to be performed by a professional either a provider or respiratory therapist because more things can go wrong when obtaining blood from an artery than a vein. That being said, today we practiced these ABG's on a simulation arm that had "blood" pulsating through it. Below you can see a picture of the radial artery being used for an ABG. Typically, this is the artery of choice. The way we can tell if we are locating an artery in contrast to a vein is that it will pulsate AND the blood will be brighter in color (that is, as long as the patient is not completely hypoxic). Unlike regular routine blood draws from veins (that have thinner more flexible walls), during an ABG the needle is held at a much greater angle (about 45-90 degrees) upon puncture. The ABG is then put on ice and sent to the lab where the pH, bicarbonate, PaCO2, PaO2 and %O2 levels are measured. With this blood gas we can tell if a patient is in respiratory acidosis, metabolic acidosis or neither. Typically, if the body is in respiratory acidosis the rest of the body will respond with compensated metabolic alkalosis (more basic in order to make up for the acidity that the lungs are creating due to a low respiratory rate, retaining too much CO2 or other issues). Since gas exchange in the lungs happens with every breath at many alveoli and capillaries, the respiratory response is much faster (minutes to hours) than the metabolic response (hours to days). The reverse can happen as well, where the body is in metabolic acidosis and then the lungs can compensate and cause respiratory alkalosis. A variety of these acid/base combinations can occur and cause the body harm; therefore, measuring these levels will help providers understand what the patient needs in order to get better. After the ABG practice, we learned how to properly splint fractures, sprains and dislocations! I have been waiting for this since day 1 in January. With simple little cases our instructor presented to us, we looked at x-rays and determined what kinds of splints helped the best with different fractures. I have helped many PA's and MD's in the ER with splinting and always wondered how they knew what type of splint to make especially when there were so many fractures or maybe even just a sprain! Even if someone presents to the ER with what looks like a sprain, clear x-ray and some swelling--- splint them and refer them to ortho! Splinting typically allows for some acute swelling so when the patient goes to their orthopedic they can protect their injury until then without completely restricting their blood flow (or worse! cause compartment syndrome). As we practiced each case, we slowly became a little better and less messy with the plaster/wrapping. I seem to have a tough time with keeping the bulk to a minimum, but I will keep practicing! Below is a picture of what an awesome job my partner did on my splints! Great work Jeff!
0 Comments
Welp, this fall seems to be very similar to the summer session in terms of how many tests we have. Overall, it looks like there is a lot less busy work, this is both good and bad. Good, in that we can focus our attention on learning the material instead of completing assignments. Bad, in a sense that we only have tests and fewer buffers for those grades. I guess we will see how it works out.
Clinical Skills Lab Aside from workload, I am most looking forward to learning the hands on lab activities like suturing, casting, ABG's etc. I have a ton of practice drawing blood from patients in the ER, but I have not done any of those other things I listed. We are paired with another student in our class to practice these skills on one another and at the nursing home. I was lucky enough to be paired with a student who has a ton of clinical experience so that he can teach me more things than I can simply read in the text book! Health Policy: Class with First Year Medical Students We also have another new combined class with the medical students. They are first year, fresh minded students who are required to work with us to help them learn more about our profession as well as us learn from them. Many medical students do not know much about PA's or that PA's are even at AMC, so this class is a passive way of making them all aware of what PA's are capable of. It will show them that we are just as knowledgeable, and if not, have more experience than them in many fields of medicine. Today we met with our small groups and got to know some of the students. The "small groups" were made up of 15 people! With such a large group it can be hard to get things initiated or even function well due to so many different personalities and intellects. Luckily, our group was extremely welcoming and there seemed to be no abrasive personalities from the PA students or the med students. This class in general is designed around a debate focus. We work with them to present one side to an answer of a question that is subject to cause conflict in the work place. We did something very similar to this in our ethics class back in the spring semester, so hopefully we will be able to bring unique skills to our small groups. Different Faculty This fall, unlike the summer, it looks like we have A LOT more faculty teaching the classes. In the summer and spring, many of the instructors overlapped on classes so on some days we had one lecturer for all the classes. It was hard on the lecturer and on us because there was no change in pace, tone or scenery. This fall it looks like we will constantly be seeing all the faculty in the classroom. I'm guessing we will get closer to the other faculty that we have not really gotten to know yet. During our time here at AMC, we, as PA students, the medical students, nurse anesthesiology students and others learn from donors' bodies as part of anatomy, surgery and other procedures. Over 300 people donated themselves to our program this year. Our PA class was fortunate enough to have benefited from 7 of them. Every year, AMC hosts a memorial ceremony to the families of those generous people who donated themselves to the future of medicine. At this ceremony we can meet the family members of those donors and maybe even get to know more about the donor. This is a great way to also thank the families for allowing this to happen, it is very difficult at the time of someone's death to allow for this and prolong the grieving process so we are very grateful and fortunate that we can learn from these donors. This year was unique in that Dr. Crone was asked to have a PA student read the names of some donors during the memorial service. (since I check my email every 3 seconds,) I replied quickly to him and offered to take that position. It was amazing to see how many people came out to the service that day to remember their loved ones. It was even more amazing that we had over 300 donors who knew about this program and offered themselves up at the end of their lives. As a student and future PA, I could not be more grateful that I had the opportunity to learn from them. They too were my teacher.
After more hours of studying than I can even comprehend, we all made it through the summer term! Rumor is we are the first class to do that in a couple of years! :) This summer term made me realize that it is possible, and we will all be PA's.
Some things I noticed about the summer term: The hardest part is just the pace and the amount of information. Constantly studying and cramming as much information in my head as fast as I could made me mentally tired most days. Unlike the spring term where I went for a run nearly every day, I did not have time/energy to do that during the summer term. Hopefully this fall term will be more conducive to a fitness lifestyle. Looking back....the tests weren't that bad. Our class average was about 88-90 on most exams and at the lowest maybe around mid 80's on some final exams. Granted, we did have to study a lot in order to get those grades, but hard work totally pays off. I personally noticed, for the most part, when I slacked on my study grind my grade reflected what I deserved, but when I studied and memorized correctly I did much better. Sometimes, no matter how much I studied, I would plateau out at a certain grade. Many people who I studied with would come out of an exam stating, "even if I had more time, I wouldn't have done much better or worse." Because you cannot possibly study every ounce of information and will need to use your thinking skills to figure things out on test day. Memorizing requires more brain power than understanding. I knew this before but this was exceptionally true, for me at least, this summer term. When there were big concepts and trends among diseases/conditions, I could learn the material so much easier with only some thought. For this type of material it also meant that I did not have to memorize much and could just figure things out on the day of the test. When I tried to memorize things, it took a shorter time to study but it made me EXTREMELY TIRED. Nevertheless, when I forced myself to memorize things I usually remember them much longer than just "figuring it out." All this work memorizing creates a great foundation for our career. I mean after all, it is called "Fundamentals of Clinical Medicine" for a reason. Congrats to the PA Class of 2017! We survived the summer term! It wasn't easy but it wasn't awful. We will take on the fall term together and be PA's before we know it! |
**As many of you can tell, I graduated AMC's program in May of 2017. Current plan is to start a new blog related to my Fellowship after PA school. Stay tuned for the link and updates :)**
Lindsey the
|